PROSTATITIS
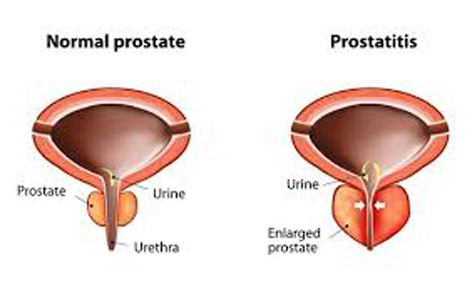
Prostatitis is a frequently painful condition that involves infection of the prostate or inflammation of the prostate and sometimes the areas around the prostate.
Prostatitis can be an acute illness or a chronic condition, The NIH consensus definition and classification of prostatitis is:
- Acute bacterial prostatitis: Caused by a bacterial infection and it typically starts suddenly and may include flu-like symptoms. It is the least common of the four types of prostatitis.
- Chronic bacterial prostatitis: Described by recurrent bacterial infections of the prostate gland. Between attacks, the symptoms might be minor or the patient may even be symptom free, however it can be difficult to treat successfully.
- Chronic prostatitis/chronic pelvic pain syndrome: Most cases of prostatitis fall into this category; however, it is the least understood. Chronic prostatitis/chronic pelvic pain syndrome can be described as inflammatory or non inflammatory, depending upon the presence or absence of infection-fighting cells in the urine, semen, and prostatic fluid. Often no specific cause can be identified. The symptoms can come and go or remain chronically.
- Asymptomatic inflammatory prostatitis: This condition is often diagnosed incidentally during the work-up for infertility or prostate cancer. Individuals with this form of prostatitis will not complain of symptoms or discomfort, but they will have the presence of infection-fighting cells present in semen/prostatic fluid.
The prostate gland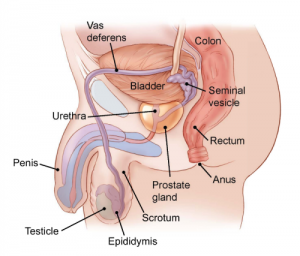
The prostate gland is part of the male reproductive system, and it is a walnut-sized gland found in men that is located below the bladder and in front of the rectum. It surrounds the urethra, the tube through which urine and semen exit the body. Its main function is to produce seminal fluid in order to transport sperm through the urethra.
Causes of Prostatitis
The causes of prostatitis differ depending on the type.
Chronic prostatitis or chronic pelvic pain syndrome. The exact cause of chronic prostatitis/chronic pelvic pain syndrome is unknown. Researchers believe a microorganism, though not a bacterial infection, may cause the condition. This type of prostatitis may relate to chemicals in the urine, the immune system’s response to a previous urinary tract infection (UTI), or nerve damage in the pelvic area.
Acute and chronic bacterial prostatitis. A bacterial infection of the prostate causes bacterial prostatitis. The acute type happens suddenly and lasts a short time, while the chronic type develops slowly and lasts a long time, often years. The infection may occur when bacteria travel from the urethra into the prostate
Nerve damage in the lower urinary tract, which can be caused by surgery or trauma to the area, might contribute to prostatitis not caused by a bacterial infection. In many cases of prostatitis, the cause isn’t identified.
Symptoms of Prostatitis
Each type of prostatitis has a range of symptoms that vary depending on the cause and may not be the same for every man. Many symptoms are similar to those of other conditions.
Chronic prostatitis/chronic pelvic pain syndrome. The main symptoms of chronic prostatitis/chronic pelvic pain syndrome can include pain or discomfort lasting 3 or more months in one or more of the following areas:
- the central lower abdomen
- between the scrotum and anus
- the penis
- the lower back
- the scrotum
Pain during or after ejaculation is another common symptom. A man with chronic prostatitis/chronic pelvic pain syndrome may have pain spread out around the pelvic area or may have pain in one or more areas at the same time. The pain may come and go and appear suddenly or gradually. Other symptoms may include
- a weak or an interrupted urine stream.
- pain in the penis during or after urination.
- pain in the urethra during or after urination.
- urinary urgency—the inability to delay urination.
- urinary frequency—urination eight or more times a day. The bladder begins to contract even when it contains small amounts of urine, causing more frequent urination.
Acute bacterial prostatitis. The symptoms of acute bacterial prostatitis come on suddenly and are severe. Men should seek immediate medical care. Symptoms of acute bacterial prostatitis may include
- urinary urgency
- urinary frequency
- a burning feeling or pain during urination
- pain in the genital area, groin, lower abdomen, or lower back
- fever
- chills
- nocturia—frequent urination during periods of sleep
- nausea and vomiting
- urinary retention—the inability to empty the bladder completely
- a weak or an interrupted urine stream
- body aches
- trouble starting a urine stream
- a UTI—as shown by bacteria and infection-fighting cells in the urine
- urinary blockage—the complete inability to urinate
Chronic bacterial prostatitis. The symptoms of chronic bacterial prostatitis are similar to those of acute bacterial prostatitis, though not as severe.Chronic bacterial prostatitis often develops slowly and can last 3 or more months. The symptoms may come and go, or they may be mild all the time. Chronic bacterial prostatitis may occur after previous treatment of acute bacterial prostatitis or a UTI. The symptoms may include
- urinary urgency
- urinary frequency
- urinary retention
- a weak or an interrupted urine stream
- painful ejaculation
- a burning feeling or pain during urination
- pain in the genital area, groin, lower abdomen, or lower back
- nocturia
- trouble starting a urine stream
- urinary blockage
- a UTI
Diagnosis
People with symptoms of prostatitis should see a doctor. Bacterial prostate infections can spread, so anyone with symptoms of an infection should seek medical attention as soon as possible.
To diagnose prostatitis, a doctor will usually begin by taking the person’s medical history. They may also perform a rectal exam.
During a rectal exam, a doctor inserts a finger into the person’s rectum to check the prostate for swelling and inflammation. They may also look for signs of infection, such as discharge from the penis or swollen lymph nodes.
If a doctor suspects the problem is due to a bacterial infection, they may recommend antibiotics. If symptoms do not improve following antibiotic treatment, or there are no signs of an infection, other tests might be necessary, such as:
- urine analysis, semen, or blood testing to look for signs of infection or other prostate issues
- a prostate biopsy, where a doctor uses a needle to remove a small sample of tissue from the prostate for analysis
- an ultrasound of the prostate or urethra
- a cystoscopy, where a doctor uses a small scope to look inside the bladder or urethra
TREATMENT
Treatment is dependent on the causative organism. Systemic herbal antibiotic therapy is chosen if the infecting organism is bacteria.
Supportive therapy includes bed rest, fluid intake, and administering herbals with analgesic and antipyretic properties. sitz baths and stool softeners are also administered if necessary.
Diet therapy may include avoiding substances that irritate the bladder. Example of bladder irritating substances are alcohol, citrus juices, caffeinated beverages and food, and spicy or hot foods.
Increasing fluids intake encourages frequent urination that help flush the bacterial from the bladder.
Regular massage of the prostate is done for symptomatic chronic prostatitis. Regular ejaculation may help promote drainage of prostatic secretions.
Plants with anticholinergic and analgesic activity may help relive nonbacterial prostatitis symptoms.
Plants Commonly Used In Ghana For The Management Of Prostatitis
Plants commonly used in the treatment/management of prostatitis in may include:
Secrinega virosa
Ageratum conyzoides
Croton membraneous
Alchornea cordifolia
Bambusa vulgaris
Zanthoxyllum zanthoxyloides
Mormordica charantia
Spathodea campatulata
Phyllanthus fratenus
Reference
Prostatitis. https://www.mayoclinic.org/diseases-conditions/prostatitis/symptoms-causes/syc-20355766 Accessed June, 2019
Prostatitis: inflammation of the prostate. https://www.niddk.nih.gov/health-information/urologic-diseases/prostate-problems/prostatitis-inflammation-prostate Accessed June, 2019
Prostatitis_(inflammation_of_the_prostate_gland ) Symptoms, Causes, Treatment, and Cure. https://www.medicinenet.com/prostatitis_inflammation_of_the_prostate_gland/article.htm Accessed June, 2019
Causes and treatment of chronic prostatitis. https://www.medicalnewstoday.com/articles/322457.php Accessed June, 2019
Ghana Herbal Pharmacopoeia (1992), 201. The Advent Press: Accra, Ghana.
Mshana, N.R., Abbiw, D.K., Addae-Mensah, I., Ahiyi, M.R.A. et al (2000). Traditional medicine and pharmacopoeia. Contribution to the revision of Ethnobotanical and Floristics Studies of Ghana. Organisation of African Unity/Scientific, technical and research committee.